Diabetes management is a must know-how in every diabetic’s life to ensure the patient avoids or delays as much as possible any complications.
Diabetes defines a metabolic disorder that can have multiple effects and is identified by modifications in the metabolism in regards to carbohydrates, lipids, and proteins. This leads to deficiency in insulin secretion, insulin resistance, or both and which has as a defining element of high blood glucose values.
The whole world is facing a type 2 diabetes pandemic, due to the modern way of life, the aging of the population, the urbanization, which results in changes in diet, the adoption of a sedentary lifestyle, and the development of obesity.
The prevalence of diabetes differs significantly depending on the population studied, age, sex, socio-economic status, and lifestyle.
The predictions for 2025 are worrying and according to the American Diabetes Association(ADA), the prevalence of diabetes will reach 9%. An important element that led in recent years to the increasing incidence of the disease has been followed by increased awareness of the population and the improvement of diagnostic methods.
However, there are at least 30% of cases of undiagnosed type 2 diabetes. The impact of diabetes on the population is enormous due to chronic (mainly cardiovascular) complications that it can generate.
The chronic complications once they appear, decrease the quality of life, functional capacity, patient autonomy, increase the number of hospitalization days, medical consultations, and medication expenses.
At the same time, the diabetic patient gradually becomes disinterested in the family or career. It also records a doubling of the mortality rate, which in the range of 70- 80% is caused by cardiovascular complications.
Reducing these serious consequences of diabetes is possible through diabetes management:
- early detection
- active use of people with diabetes in the population
- groups at risk,
- treating patients once diagnosed according to therapeutic protocols based on international evidence
- preventing the onset of chronic complications and their aggravation through the systematic screening of complications and treatments specific for cases of aggravation of chronic complications, in collaboration with specialists cardiologists, nephrologists, neurologists, ophthalmologists.
- Care of diabetic patients also requires psychological assistance, improved family integration, socially and professionally.
- Care for diabetic patients should be performed by a multidisciplinary team in which its coordination is the responsibility of the specialist diabetologist but in which an important role is played by the diabetic patient who must actively participate in all decisions related to its care and the subgroup population it represents.
The cost of diabetes, direct and indirect, is extremely high, reaching up to to 10% of the health budgets of many countries . The cost of diabetes is rising 3-5 times if micro and / or macro cardiovascular chronic complications occur.
The bottom line is that the prevention of chronic complications of diabetes improves the clinical-therapeutic and psycho-social impact and reduces the cost of the disease for both the patient, the patient’s family and the medical care involved.
The clinical stages of diabetes
The clinical stages reflect the fact that the condition goes through several stages:
- The normoglycemic stage. This classification proposed by the World Health Organization(WHO), includes the normoglycemic stage as the first stage in the evolution of diabetes in people in which there is evidence of the pathological process. Normal glucose tolerance is defined by a fasting blood glucose value <110 mg/dl and 2 hours after administration of 75 g glucose <140 mg/dl.
- Modifications of glycemic regulation – deterioration of glucose tolerance and deterioration of basal blood glucose represent an intermediate stage between normal tolerance to glucose and diabetes.
A fasting blood glucose value> 110 mg/dl but <126 mg/dl is considered to deteriorate basal blood glucose and a blood glucose value of fasting <126 mg/dl and 2 hours after administration of 75 g glucose between 140 mg/dl and 199 mg / dl define impaired glucose tolerance.
3. Diabetes. Patients diagnosed with diabetes, from a clinical point they are classified into:
- those who need insulin therapy in survival
- those who require insulin therapy to obtain a metabolic control
- those who do not require insulin therapy.
In 2009 a committee of international experts recommended the use of glycosylated hemoglobin(A1C), in diagnosing diabetes mellitus at a value of ≥ 6.5%, a recommendation adopted by the American Diabetes Association since 2010.
Type 1 diabetes screening
In general, type 1 diabetes starts with acute symptoms and high values of blood sugar levels, in most of the cases being diagnosed soon after the onset of hyperglycemia.
A comprehensive test for the detection of specific antibodies in all asymptomatic patients can not be currently recommended as a way to detect patients at risk. These tests may be appropriate in people at high risk and hyperglycemia, respectively transient history or hereditary history of diabetes.
Type 2 diabetes screening
The role of screening methods in the diagnosis of type 2 diabetes in asymptomatic individuals should be considered in overweight adults or obese people who have one or more risk factors that will be mentioned subsequently.
In the absence of risk factors, the screening will be performed after the age of 45 years. Standard recommendations:
- basal blood glucose test is recommended: age> 45 years, sedentary lifestyle, race/ethnicity characterized by an increased frequency of this condition
- relatives with diabetes diabetes
- the birth of a child> 4kg or a diagnosis of gestational diabetes
- overweight or obese people
- syndrome of polycystic ovaries, hypertension (blood pressure values > 140/90 mmHg), history of vascular distress, HDL-cholesterol values <35 mg / dl and / or triglycerides ≥250 mg / dl
It is recommended for people without risk factors that the blood glucose test is performed once every five years after the age of 18 years and once every 3 years after the vast 45 years.
If the person has one or 2 risk factors and increased blood sugar<126 mg it is recommended that they take the tolerance oral glucose test(TTGO), with 75 g glucose. TTGO is performed in the morning, at rest, after at least 8 hours of rest (post-night), and in the conditions in which the person consumed at least 250g carbohydrates/day in the previous 3 days.
Investigations for type 2 diabetes in children
Standard recommendations: overweight children will be investigated (body mass index> 85th percentile by age and sex, height-adjusted weight> 85th percentile or weight> 120% of ideal weight) having two of the following risk factors: family history of type 2 diabetes in relatives, maternal history of diabetes or gestational diabetes, race/ethnicity characterized by an increased frequency of this condition, signs of insulin resistance or conditions associated with insulin resistance, maternal history of gestational diabetes. Testing should begin at the age of 10 or at puberty.
Prevention and delay of the onset of type 2 diabetes
Deterioration of glucose tolerance and increased blood sugar were certain categories with an increased risk of diabetes. Randomized studies controlled showed that for patients at high risk of diabetes there are adequate interventions that are able to reduce the rate of onset of diabetes. The prevention strategy aims to control manageable risk factors in general and in people at high risk of developing diabetes. The prevention program includes 3 stages:
- identification of people at high risk of developing diabetes
- risk quantification
- prevention methods.
People with a high risk of developing type 2 diabetes need to be included in programs aimed at changing the style of life including moderate weight loss and regular physical activity.
Counseling during follow-up seems important for the success of therapy. Proper follow-up of the patient with diabetes can only be achieved in a multidisciplinary team, a team that includes doctors, nurses, nutritionists, pharmacists, and mental health specialists with experience in the problem of diabetes.
Lifestyle management
Patients with type 2 diabetes are mostly overweight or obese and generally have an unhealthy lifestyle (unhealthy eating habits, sedentary lifestyle) which contributed, along with other factors, to the onset of the condition. Therefore, it is necessary to identify immediately after diagnosis ways of intervention on lifestyle.
By improving the style of life we aim to achieve and maintain the ideal body weight, decrease glycemic values, normalize uric acid values (or bringing it as close as possible to normal), maintaining optimal values of blood pressure, sometimes in combination with specific medication. Smoking is an independent cardiovascular risk factor, therefore we will insist on quitting smoking and alcohol consumption.
It is recommended to change previous eating habits and provides access to a dietitian. The diet is individualized according to age, sex, height, weight, degree of physical activity, preferences, local tradition, and level of culture. Carbohydrate intake monitoring is an essential part of the strategy for achieving optimal glycemic control.
Restrict alcohol consumption to one alcoholic beverage per day for women and 2 alcoholic beverages for men.
Saturated fat intake should be <7% of total caloric intake. The intake of trans lipids will be reduced to a minimum.
Protein intake is restricted to 0.8-1 g / kg / day in adults.
Exercise is introduced gradually, depending on the abilities of each individual; prolonging the duration and increasing the frequency is encouraged in physical activity (where necessary) up to 30-45 min/day, 3-5 days/week, or 150 min./week.
In the absence of other counter-indications, people with type 2 diabetes should be encouraged to practice resistance training three times a day week.
Quitting smoking. Epidemiological studies have provided convincing documentation on the causal link between smoking and health risk. Studies performed on diabetic patients constantly showed an increased risk of cardiovascular disease and premature death in smokers.
Smoking is also associated with the premature onset of microvascular complications and could play a role in the onset of type 2 diabetes.
Recommended blood sugar values
The recommended targets by the ADA for adults are HbA1c <7%, preprandial capillary blood glucose 70 – 130 mg/dl, postprandial capillary blood glucose <180 mg/dl. Regarding glycemic control in women with gestational diabetes, it is recommended to reduce glucose levels in maternal whole capillary blood at preprandial ≤ 95 mg/dl and ≤ 140 mg/dl 1 hour after meals and respective 120 mg/dl, respectively, at 2 hours after meals. For women with type 1 or 2 diabetes who become pregnant, ADA recommends the following therapeutic targets in the conditions in which they can be obtained without excessive hypoglycemia: preprandial glycemia, at bedtime and during the night 60 – 99 mg/dl, the maximum blood glucose value postprandial 100 -129 mg/dl, HbA1c <6%. Monitor glycemic control using A1c performed at least twice a year in patients who meet the therapeutic objectives and have stable metabolic control. A1c will be determined quarterly in patients whose therapy has been modified or which do not meet the objectives of glycemic control. Less stringent target values of A1c are appropriate for people with a history of severe hypoglycemia, limited life expectancy or severe complications, significant comorbidities, or when the objectives are difficult to be achieved in the conditions in which intensive education measures have been implemented repeated counseling. The ADA states the fact that the glycemic target must reflect an agreement between the patient and the clinician. The goals of glycemic control in children are according to ADA: infants and preschoolers, target values (limits) of blood glucose before meals 100 – 180 mg / dl, at bedtime, overnight 110 – 200 mg / dl, HbA1c <7.5%, schoolchildren 90 – 180 mg / dl, HbA1c <7.5, 100 – 180 mg / dl, HbA1c <7.5% adolescents and young adults 90 – 130 mg / dl, 90 – 150 mg / dl, HbA1c <7.5%. The association recommends that in conditions of severe episodes of hypoglycemia modification of the patterns of treatment, including setting higher blood glucose target values is an absolute indication. Less stringent A1c is preferred in patients where the disease advanced also with atherosclerotic cardiovascular disease, patients at major cardiovascular risk. In the case of HbA1c values> 7.5% at two quarterly determinations at patients with type 2 diabetes, prescribing oral medication and with a low degree of validation, the use of these medications becomes unjustified.
Self-monitoring of blood glucose
The self-control of blood sugar is an integral part of the treatment strategy for both insulin-treated and patients treated with s oral medication.
In the process of therapeutic education, self-monitoring is essential for proper adjustment of insulin doses in different situations, for grading physical effort or food intake, all these to achieve and maintain therapeutic goals.
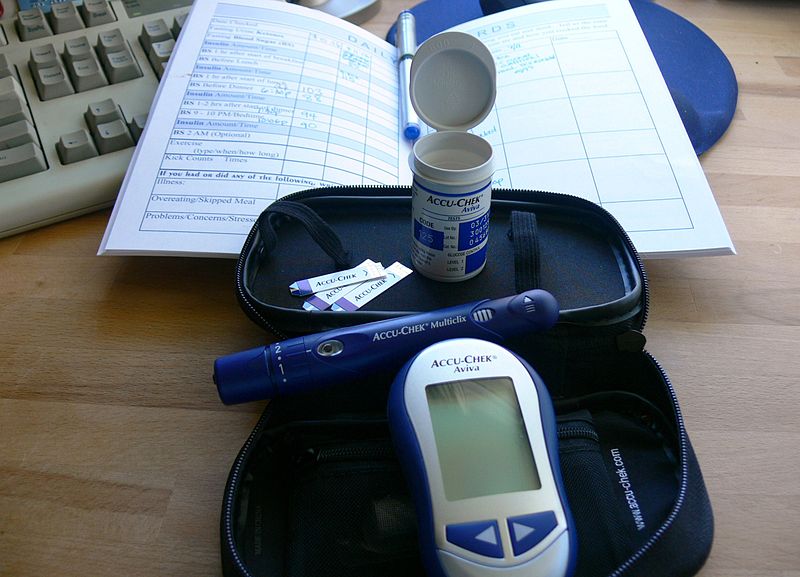
Self-monitoring of blood glucose (using the glucometer) is required for insulin-treated patients with diabetes and women with gestational diabetes.
Self-monitoring in patients with diabetes treated with oral medication, can be useful to provide information about hypoglycemia, may show glycemic changes due to changes in medication or lifestyle, and can monitor changes that occurred during intercurrent diseases.
Self-monitoring is beneficial if people with diabetes are trained to perform self-testing, to record data, to understand their significance, and to intervene in the therapeutic scheme or to address to a specialist.
HYPOGLYCEMIA
Hypoglycemia is the main limiting factor in managing the glycemic index of type 1 diabetes and type 2 diabetes. The standard recommendations are glucose (15 – 20 gr) is the preferred treatment in people conscious with hypoglycemia. Treatment should be repeated if, at 15 minutes after glucose administration, blood glucose levels remain low.
Once blood sugar levels return to normal the person should consume a snack or meal to reduce the risk of hypoglycemia.
Glucagon is recommended to be prescribed to all patients at risk of significant severe hypoglycemia.
Diabetes management means you need to understand the disorder first. Then eliminate the bad lifestyle habits, if you smoke – stop it, manage your diet, monitor blood sugar levels, and practice sports. If you manage your diabetes, then your diabetes won’t manage your life.
